
Ovarian, fallopian tube, and peritoneal malignancies are collectively, "ovarian cancer". The malignancies have similar treatment because they are closely related to one another.
Certain cancers start when healthy cells in these regions transform and proliferate out of control to produce a mass known as a tumour. A tumour may be benign or malignant. Malignant refers to the ability of a cancerous tumour to develop and metastasize to different body regions. If a tumour is benign, it can enlarge but won't spread.
An abnormal growth of tissue on the surface of the ovary is an ovarian cyst. It can happen during a typical menstrual cycle and typically goes away on its own. Cancer is not present in simple ovarian cysts.
According to recent studies, high-grade serous cancers account for the majority of ovarian/fallopian tube cancers, and in most cases, the disease begins at the tip, or outer end, of the fallopian tubes. It then spreads to the ovaries' surface and has the potential to expand further.
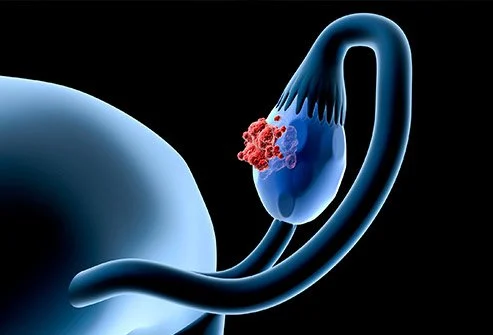
Given this new information, several medical professionals advise against tying or banding fallopian tubes for contraception (to prevent future pregnancy) to reduce the risk of ovarian/fallopian tube cancer. When a patient is having surgery for a benign ailment and does not wish to become pregnant in the future, some doctors additionally advise fallopian tube removal. This approach might lessen the likelihood that these malignancies would spread in the future.
Also Read: Is Ovarian Cancer Curable?
Under a microscope, the majority of these illnesses resemble one another because the ovaries' surfaces, the fallopian tubes' lining, and the peritoneum's covering cells are composed of the same sorts of cells. Rarely, peritoneal cancer can appear after the removal of the ovaries and fallopian tubes. Some peritoneal malignancies, like ovarian cancer, can start in the fallopian tubes and progress from the tube's end into the peritoneal cavity.
Your overall health, the stage of the cancer, the length and intensity of therapy, and other variables all affect how your physical health will change.
Discuss your feelings frequently with your medical staff. If you experience any side effects while taking paclitaxel, such as peripheral neuropathy, it's vital to inform your doctor right away because it cannot go away when you discontinue the medication. Knowing how you are feeling will help them find strategies to alleviate or manage your side effects, making you feel more at ease and possibly preventing any side effects from getting worse.
Keeping track of your side effects can make it simpler for you to communicate any changes to your medical staff. Sometimes, following a course of treatment, adverse effects may persist. Physicians refer to this as long-term adverse effects. Late effects are side effects that manifest months or years after therapy. An essential component of survivorship care is treating late symptoms and long-term side effects.
Following a cancer diagnosis, you may have emotional and social repercussions. This might entail managing your stress levels or coping with a range of emotions, such as grief, anxiety, or rage. Sometimes it might be tough for folks to tell their loved ones how they feel. Some people have discovered that speaking with an oncology social worker, counsellor, or clergyperson can help them come up with better-coping mechanisms and cancer-related communication strategies. Speaking with your peers, including those who have been diagnosed with ovarian cancer, can also be helpful. It is crucial to discuss your emotional well-being with your doctor because anxiety and sadness are prevalent during cancer treatment and can be effectively managed.
The cost of cancer therapy might be high. For those who are dealing with cancer and their families, it could be a cause of stress and anxiety. Many patients discover they have additional, unforeseen fees related to their care on top of the cost of their therapy. Some people are unable to follow or complete their cancer treatment plan due to the high cost of medical care. This could endanger their health and result in future expense increases. Financial worries should be discussed with a member of the patient and family's healthcare team.
Some groups of people experience different rates of new cancer cases and experience different outcomes from their cancer diagnosis. These differences are called cancer disparities. Disparities are caused in part by real-world barriers to quality medical care and social determinants of health, such as where a person lives and whether they have access to food and health care. Cancer disparities more often negatively affect racial and ethnic minorities, people with fewer financial resources, sexual and gender minorities (LGBTQ+), adolescent and young adult populations, older adults, and people who live in rural areas or other underserved communities.
Also Read: Ovarian Cancer Follow-up Care
If you are having difficulty getting the care you need, talk with a member of your healthcare team or explore other resources that help support medically underserved people.
Discuss potential side effects with your doctor before beginning therapy. Ask:
Tell your medical provider right away if you have any side effects both during and after your therapy. Even if you don't believe the side effects are substantial, tell them. The financial, social, emotional, and physical repercussions of cancer should all be included in this conversation.

When someone has ovarian/fallopian tube cancer, family and friends frequently play a crucial part in their care. This is what it means to be a caretaker. Even if they are far away, caregivers can support the sufferer physically, practically, and emotionally. It can be exhausting and emotionally taxing to be a caretaker. Taking care of oneself is one of the most crucial jobs for caregivers.
A caregiving plan can keep caregivers organised and show them where they can assign work to others. Asking the medical staff how much assistance will be required during and after treatment at home and with daily duties may be useful.
Elevate your Journey with Enhanced Immunity & Well-being
For personalized guidance on cancer treatments and complementary therapies, consult our experts atZenOnco.ioor call+91 9930709000
Reference: